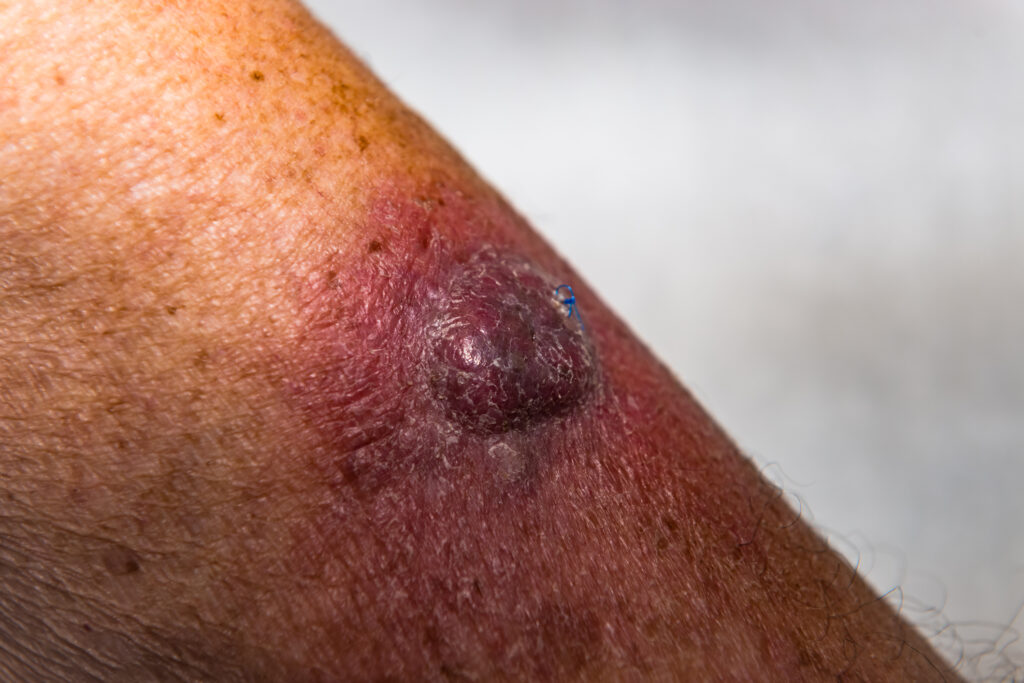
Researchers at the Perelman School of Medicine at the University of Pennsylvania have developed a topical cream designed to treat cutaneous squamous cell carcinoma (cSCC), a common form of skin cancer, by activating immune responses within the skin. As described in research published in the Journal of Clinical Investigations, the therapy works by inhibiting lysine-specific demethylase 1 (LSD1), an enzyme that suppresses immune-activating pathways in epidermal cells. By blocking this enzyme, the cream stimulates communication between skin cells and the immune system enabling it to attack tumor cells.
“What’s striking is that a simple topical cream can use the skin’s own machinery to recruit and activate immune cells that attack tumors,” said senior author Brian C. Capell, MD, PhD, an assistant professor of dermatology at UPenn. “We are carrying out some more studies to refine the formulation this coming year, and we hope to begin a Phase I clinical trial in the next 1-2 years. Ideally, this cream could be used directly on cancerous and precancerous spots.”
Cutaneous squamous cell carcinoma is one of the most common cancers, with about one million Americans diagnosed each year. While most tumors can be treated successfully with surgery, the cancer can spread after initial treatment and become life-threatening. Further complicating treatment for those patients whose cancer spreads, is the development of precancerous lesion across the skin that could require multiple procedures that may not be well tolerated in older or immunocompromised patients.
As described by the researches, the topical cream works by targeting LSD1, also known as KDM1A, an enzyme involved in regulating gene expression through epigenetic mechanisms. LSD1 normally removes methyl groups from specific histone marks associated with gene activation, thereby repressing certain genetic programs. In skin cells, this repression includes pathways connected to immune activation.
“Lysine-specific demethylase 1 (LSD1; KDM1A) orchestrates context-dependent chromatin programs, yet its role in epithelial immunity remains largely unknown,” the researchers wrote. By inhibiting LSD1 in the skin, the treatment blocks the molecular brake suppressing immune signaling, to allow epidermal cells to initiate immune responses to attack tumors.
To investigate whether inhibiting LSD1 could help boost immune response, the team formulated a low-dose topical LSD1 inhibitor and tested it in two preclinical models of cutaneous squamous cell carcinoma. The experiments included genomic mapping, chromatin profiling, and single-cell spatial analyses to track changes in gene expression and immune signaling after LSD1 inhibition. Data from this work showed that LSD1 binds to enhancer regions of the genome associated with immune and retinoid signaling pathways. When the enzyme was inhibited, genes involved in these pathways became activated.
Single-cell spatial analyses further showed that specific subsets of keratinocytes initiated retinoic acid signaling that helped recruit dendritic cells and activate CD4⁺ T cells. The study demonstrated that these immune cells were required for tumor suppression. Blocking retinoic acid signaling reversed many of the molecular changes induced by the cream, and eliminating CD4⁺ T cells removed its anti-tumor effects, indicating that immune activation played a central role in the treatment’s mechanism.
The current study builds on earlier research that LSD1 can influence immune signaling and may enhance immunotherapy responses in other tumor types, including breast, cervical, and colon cancers. Prior to this research, however, its role in activating immune response in the skin had not been characterized.
These new findings help define the broader biological role of LSD1 in skin biology. “Thus, from embryonic development through cancer progression, LSD1 functions as a master regulator of skin biology through coordinated control of differentiation, retinoid, and immune signaling networks,” the researchers wrote.
Future research will seek to refine the skin cream’s formulation and will evaluate safety and efficacy in early stage, in-human trials. The UPenn team will also examine whether systemic delivery of LSD1 inhibitors in oral or injectable forms, could enhance the effectiveness of immune checkpoint therapies in patients with advanced disease.