Results from the PRIMARY2 clinical trial show that an imaging test could significantly reduce the number of people with suspected prostate cancer who need a biopsy following inconclusive results from an MRI scan. These findings were presented today at the European Association of Urology Congress in London (EAU26).
The Phase III clinical trial evaluated the use of PSMA PET/CT scanning, a technique that involves the injection of a radiopharmaceutical targeting the prostate-specific membrane antigen (PSMA), which is overexpressed in prostate cancer cells.
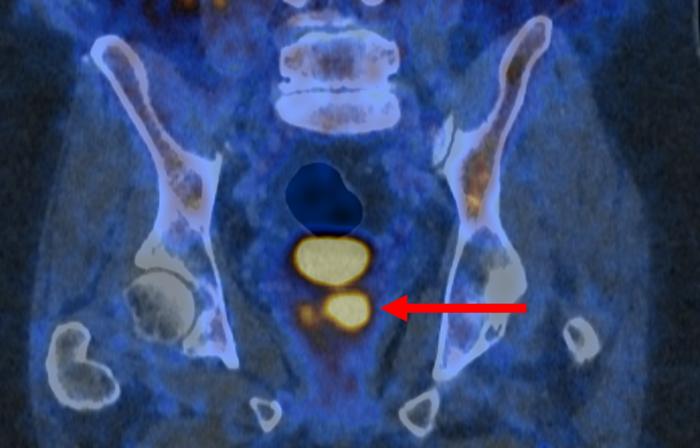
“PSMA PET/CT scanning makes prostate cancer cells light up in a remarkable way, particularly in more aggressive cancers. It’s rare to see such strong imaging that could be so powerful in the clinic,” said James Buteau, MD, nuclear medicine physician at Peter MacCallum Cancer Centre in Australia, who presented the research today at EAU26. “Incorporating this testing into clinical care could help to address the major challenge of prostate cancer overdiagnosis, which leads to at best unnecessary and at worst harmful treatment for cancers that would never cause any harm.”
All 660 participants recruited in the Australia-wide clinical trial had received results indicating a low or intermediate risk of prostate cancer based on their initial MRI scan, and carried additional risk factors such as rising PSA score or a family history of cancer. Normally, patients with this kind of profile will be referred to a routine biopsy test to either rule out or confirm the presence of prostate cancer.
Participants were randomized to either undergo a standard biopsy or a PSMA PET/CET scan. In the experimental arm, the imaging technique was used to identify which patients did not have cancer, or one with low risk or slow growth that would likely never become harmful. Those with positive scan results went on to receive a biopsy to confirm the suspected prostate cancer.
Results showed that PSMA PET/CT scanning reduced the percentage of patients without prostate cancer who received a biopsy from 44% to 22%, halving the need for this invasive procedure. This supports the use of PSMA PET/CT scans in routine practice to improve prostate cancer diagnosis and reduce the number of unnecessary biopsies performed without compromising the detection of positive cases.
Although cost and availability still limit the widespread use of this imaging technique, PSMA PET/CT scanning is becoming increasingly accessible for clinics worldwide.
“Getting told you have a risk of prostate cancer is a huge cause of anxiety and concern,” said Louise Emmett, MD, PhD, director of theranostics and nuclear medicine at St Vincent’s Hospital Sydney. “Our findings show that PSMA PET/CT after MRI offers a ‘belt and braces’ approach that can determine which people have a clinically significant cancer, and which people are at low risk and don’t need a biopsy or further testing.”